Get Providers In-Network Start Billing Sooner
Fully managed payer enrollment for hospitals, medical groups, and telehealth. Commercial, Medicare, and Medicaid — with real-time visibility from intake to approval.
50-state coverage
CAQH & NPPES managed
Live status dashboard
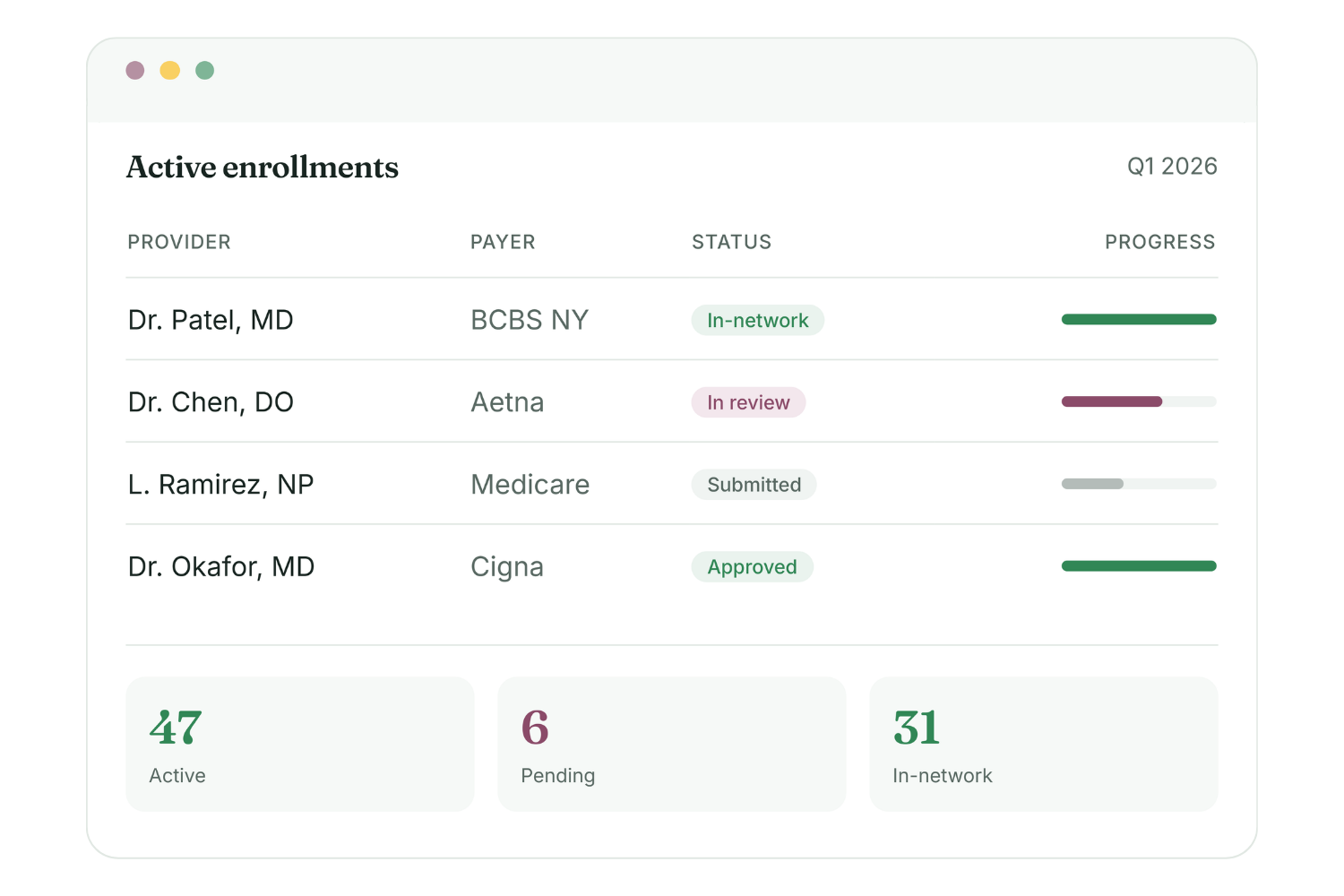
Manages
Payer Enrollment for Every Provider Type
Each provider type has unique requirements and revalidation timelines. We manage them all.
Physicians
MD/DO across all specialties.
Nurses
RNs, CRNAs, specialty nursing.
Advanced Practice
NPs, PAs, CRNPs, CNMs.
Behavioral Health
Psychiatry, LCSW, LPC, MFT.
Complete Enrollment, End to End
From application to approval — every payer, every document, every follow-up handled
Commercial Enrollment
BCBS, Aetna, Cigna, UHC, Humana — payer-specific tracking from day one.
Medicare & Medicaid
PECOS, 855I/855B, and state MCO applications run in parallel.
CAQH Management
Profiles complete, attestations on schedule. No frozen claims.
Milestone Tracking
Live status per provider, per payer, with projected go-live dates.
Group & Roster
Scaled enrollment for medical groups and health systems.
NPPES Sync
Clean upstream data — fewer information requests, faster approvals.
2x
Faster enrollment vs. in-house
58%
Reduction in administrative costs
100%
Application visibility
50
States · All payer types
From Onboarding to In-Network, Simplified
We handle every step so your providers get in-network faster, without the back-and-forth
1
Intake
Documents assessed against payer-specific requirements.
2
Data alignment
CAQH and NPPES audited so payers receive clean info.
3
Multi-payer submit
Commercial, Medicare, Medicaid in parallel.
4
Active follow-up
We chase payers — applications keep moving.
5
In-network
Effective dates confirmed, billing team notified.
Platform Built for Visibility & Control
Real-time tracking
Projected go-live dates
Revalidation lifecycle
Denial prevention
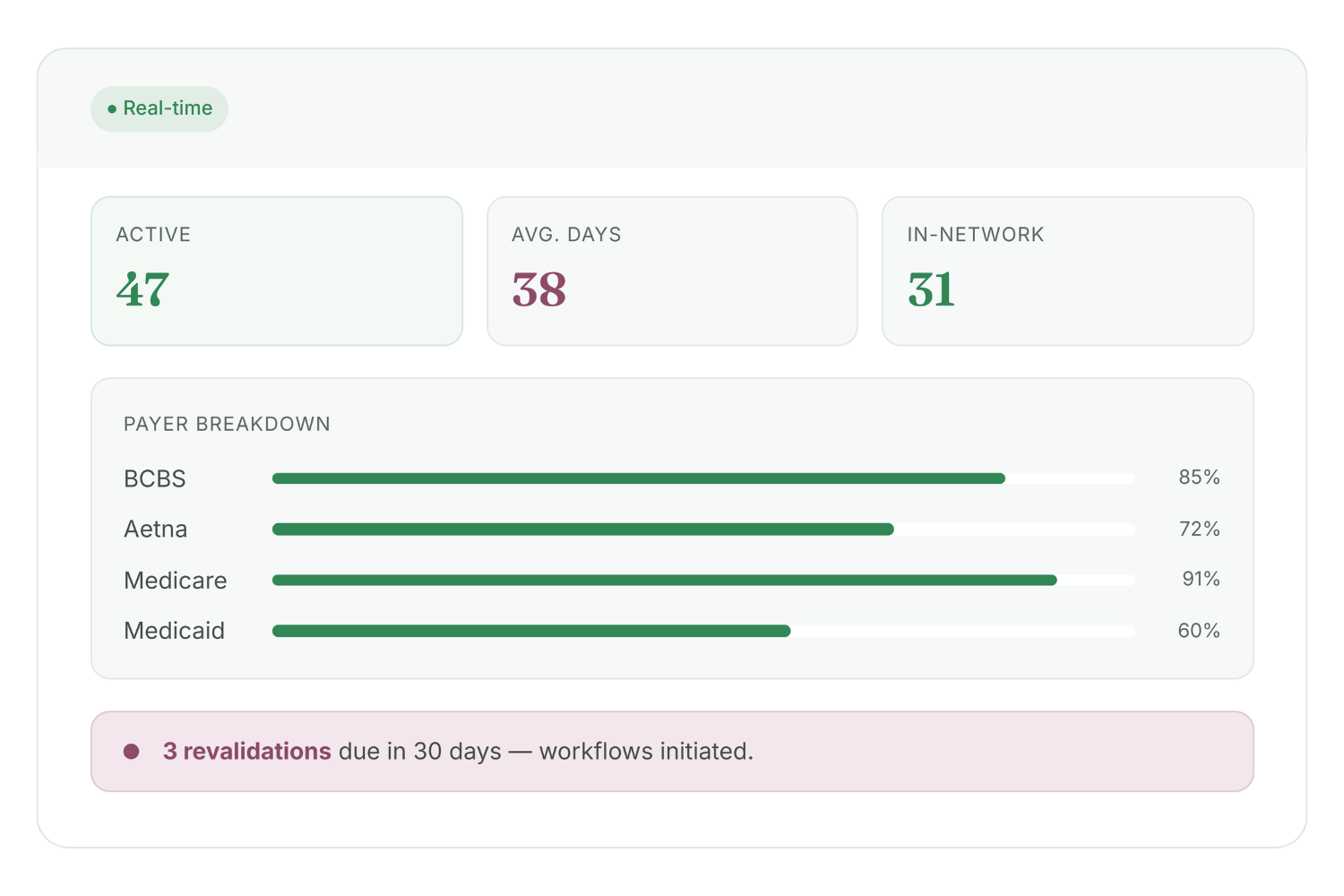
FAQ
Your Questions Answered.
How long does enrollment typically take?
Commercial enrollments usually run 60–120 days when handled reactively. With proactive follow-up, document readiness, and parallel submissions, we compress that significantly. Medicare/Medicaid timelines depend on CMS queues — we initiate simultaneously to avoid stacked delays.
Can enrollment start while credentialing is still in progress?
Yes — and most teams miss this. Many payer applications can begin in parallel with credentialing. We align both on one platform so enrollment is ready the moment credentials verify.
What happens when an application is rejected or delayed?
We catch rejections and delays in real time, diagnose the cause, and resolve them without waiting for your team to notice. Every escalation is documented in your dashboard.
Do you handle Medicaid across multiple states?
Yes — all 50 states, including MCO applications, fee-for-service, and state-specific portals. Multi-state submissions coordinated simultaneously.
Do you enroll behavioral health and APPs?
Yes — physicians, nurses, NPs, PAs, psychiatrists, psychologists, LCSWs, LPCs, MFTs. Each credential type has different requirements; we manage the nuances.
Is CAQH and NPPES management included?
Yes. CAQH ProView, re-attestation tracking, and NPPES synchronization are part of the service. Clean upstream data means faster approvals downstream.
Stop Leaving Revenue on the Table
Every day a provider isn't enrolled is revenue you can't recover.
Let's compress the timeline.






